Endocrine Disorders in Adults With End-Stage Renal Disease on Dialysis: A Review
DOI:
https://doi.org/10.14740/wjnu1036Keywords:
Endocrine alterations, End-stage renal disease, Hyperprolactinemia, HypogonadismAbstract
Background: Endocrine dysfunctions are frequent yet underrecognized complications of end-stage renal disease (ESRD), with major implications for prognosis, quality of life, and treatment. This review provides an updated synthesis of endocrine alterations in ESRD, emphasizing clinical impact, dialysis modality differences, and research needs.
Methods: A systematic search of PubMed and EMBASE identified studies published between January 1975 and January 2026, including observational studies, randomized controlled trials (RCTs), systematic reviews, and international guidelines. Evidence was synthesized across major pathways in ESRD: hypothalamic-pituitary-gonadal axis, prolactin, thyroid function, vitamin D-parathyroid hormone metabolism, and adrenal function. Particular emphasis was placed on pivotal RCTs (EVOLVE, PRIMO, OPERA, phosphodiesterase type 5 inhibitor studies) and key guidelines statements (Endocrine Society, American Thyroid Association (ATA), European Menopause and Andropause Society (EMAS), Kidney Disease: Improving Global Outcomes (KDIGO), European Renal Association–European Dialysis and Transplantation Association (ERA-EDTA), American Urological Association (AUA)).
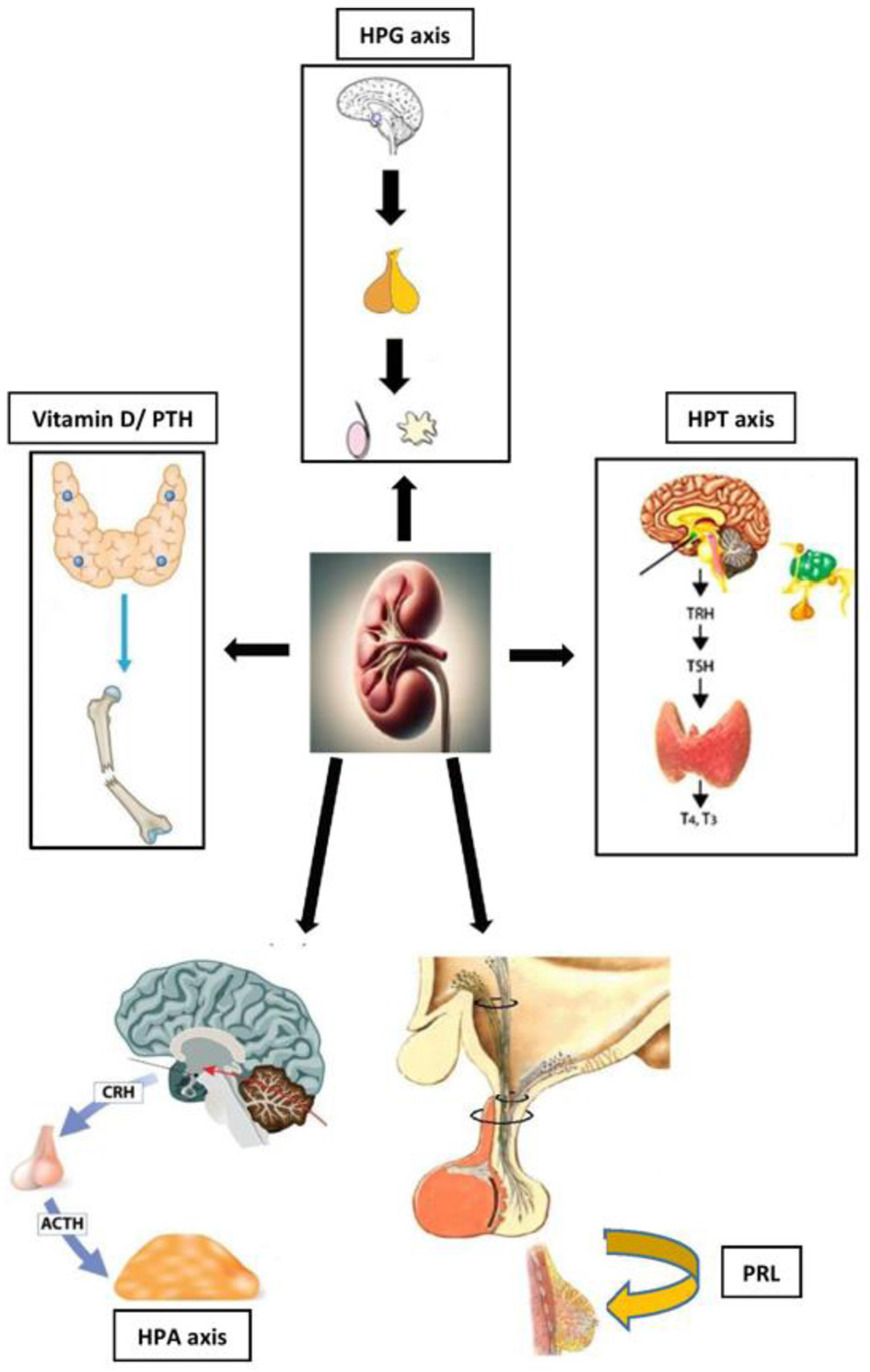
Results: Hypogonadism affects up to two-thirds of male dialysis patients, contributing to cardiovascular risk, anemia, and mortality; in women on dialysis, ovarian failure drives infertility and sexual dysfunction. Hyperprolactinemia is highly prevalent and exacerbates gonadal dysfunction, with potential cardiovascular relevance. Thyroid alterations include “low-T3 syndrome”, an independent predictor of mortality, and increased risk of subclinical and overt hypothyroidism. Chronic kidney disease-mineral and bone disorders contributes to bone disease, vascular calcification, and adverse outcomes. Dialysis modality (hemodialysis vs. peritoneal dialysis) influences endocrine stability and quality of life.
Conclusions: Endocrine disorders in ESRD are prognostically relevant and require systematic screening, tailored management, and multidisciplinary care. Current evidence is predominantly observational, underscoring the urgent need for randomized trials to establish optimal therapeutic strategies and clarify their impact on survival and cardiovascular outcomes.
Published
Issue
Section
License
Copyright (c) 2026 The authors

This work is licensed under a Creative Commons Attribution 4.0 International License.





